If you’ve ever felt a “pop” in your knee followed by stiffness or the sensation that your leg might give out, you’re not alone. Meniscus tears are among the most common knee injuries we see at RegenRx.
For years, the standard answer was surgery—simply cutting out the damaged piece. However, we now know that preserving your meniscus is vital for long-term joint health. In this post, we’ll explore what a meniscus tear really is and why regenerative medicine is changing the way we heal.
What Exactly is a Meniscus?
Think of your knee like a high-performance vehicle. Your meniscus is the shock absorber. Each knee has two C-shaped wedges of fibrocartilage (the medial and lateral meniscus) that sit between your thigh bone and shin bone. They distribute weight, stabilize the joint, and protect your cartilage from wearing down.
How Tears Happen
Meniscus injuries generally fall into two categories:
- Acute Traumatic Tears: These often happen during sports. A sudden twist or pivot while the foot is planted can cause the tissue to tear.
- Degenerative Tears: As we age, the meniscus becomes more brittle. Something as simple as squatting down to garden or stepping off a curb can cause a tear in a weakened meniscus.
The “Map” of a Tear: Types and Patterns
Not all tears are created equal. The pattern of the tear often dictates how well it can heal on its own:
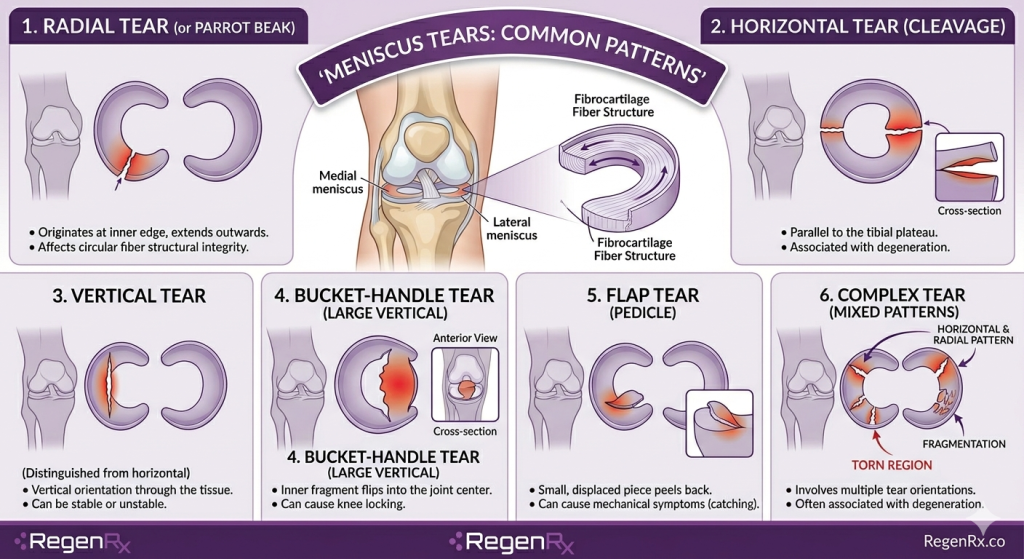
- Radial Tears: The most common; these occur in the “white zone” (the inner part) where blood flow is poor.
- Bucket-Handle Tears: A large vertical tear that can cause the knee to “lock” because the torn piece flips into the joint.
- Horizontal Tears: Often linked to degeneration and wear-and-tear over time.
- Flap Tears: An unusual pattern where a small piece of the tissue peels back and catches in the joint.
Diagnosis: How We Find the Problem
At RegenRx, we don’t just look at an image; we look at the person. Diagnosis typically involves:
- Physical Exam: We use specialized tests like the McMurray test, where we rotate the knee to check for clicking or pain.
- MRI Imaging: This is the gold standard for seeing the exact “map” of the tear.
- Dynamic Ultrasound: Unlike a static MRI, we can use ultrasound to watch your knee move in real-time, helping us see if the meniscus is stable.
Management Options
Traditionally, many patients were rushed into a meniscectomy (removing the torn part). But removing the shock absorber often leads to “bone-on-bone” arthritis down the road. Our goal is joint preservation.
Conservative Care
For minor tears, we start with the “RICE” method (Rest, Ice, Compression, Elevation) combined with specialized physical therapy to strengthen the muscles supporting the knee.
When is Surgery Necessary?
While we aim to avoid surgery, certain “unstable” tears (like a bucket-handle tear that locks the knee) may require a surgical repair (stitching it back together). Even in these cases, regenerative treatments can be used post-surgery to speed up recovery and improve the quality of the healed tissue.
Regenerative Medicine Approaches
Some patients explore regenerative medicine procedures as part of a comprehensive, non-surgical care plan for meniscus injuries. These procedures are designed to support the body’s natural healing response and are typically considered alongside rehabilitation, activity modification, and other conservative measures.
Platelet-Rich Plasma (PRP)
PRP involves drawing a small sample of the patient’s blood and processing it to concentrate platelets and growth factors. The prepared PRP is then injected into the area of concern using image guidance when appropriate.
Cell Therapy
These products contain naturally occurring growth factors, cytokines, and extracellular matrix components and may be considered in select patients as part of an individualized treatment approach.
Extracorporeal Shockwave Therapy (ESWT)
Shockwave therapy is a non-invasive modality that delivers acoustic pressure waves to targeted tissues. ESWT is commonly used in musculoskeletal medicine and may be incorporated into a broader rehabilitation strategy.
Why Choose Conservative Therapy Over Removal?
The statistics are clear: patients who keep their meniscus have a significantly lower risk of needing a total knee replacement later in life. By choosing regenerative options, you’re not just treating the pain—you’re protecting your future mobility.
Ready to get back to doing what you love? Don’t let a “pop” stop you. Contact the team at RegenRx today for a consultation and let’s see if regenerative medicine is the right path for your recovery.
Disclaimer: This blog is for educational purposes and does not constitute medical advice. Always consult with a qualified healthcare provider for a diagnosis.
Learn More About Your Options
Have questions or want to learn more about our treatments? We’re here to help. Contact our team today to discuss your options, schedule a consultation, or get answers to any concerns you may have. We look forward to guiding you on your journey to better wellness.

Written By: Ritu Patel, FNP-BC
Expert in Regenerative & Restorative Medicine

